Insuring the Nation: Government Schemes Making Protection Accessible to All
A Blueprint for Inclusion: Insurance by the People, for the People
India’s pursuit of universal insurance coverage is being significantly shaped by a series of large-scale, government-backed programs that aim to provide financial protection to underserved and vulnerable sections of society. While the private insurance sector continues to innovate with customer-centric digital products, it is the state-led initiatives that have laid the groundwork for mass-scale inclusion— leveraging technology, banking infrastructure, and administrative reach.
Pradhan Mantri Jan Arogya Yojana (PMJAY):
Among these, the Pradhan Mantri Jan Arogya Yojana (PMJAY) stands as a pioneering effort in public health insurance. Introduced in 2018 under the Ayushman Bharat mission, PMJAY is the world’s largest government-funded healthcare scheme, providing coverage of up to ₹5 lakh per family per year for hospitalization across a network of public and private hospitals. The program targets over 50 crore citizens—approximately 40% of India’s population—based on socio-economic data from the SECC 2011 database. Enrollment is automatic for eligible families (12 crore poor and vulnerable entitled families, approximately 55 crore beneficiaries) and the scheme is entirely cashless and paperless at the point of service. Its implementation is overseen by the National Health Authority (NHA), supported by a digital health infrastructure comprising Ayushman Bharat Health Accounts (ABHA), e-cards, and hospital management systems. To date, over
₹75,000 crore worth of treatments have been administered through more than 26,000 empanelled hospitals nationwide.

How it Works:
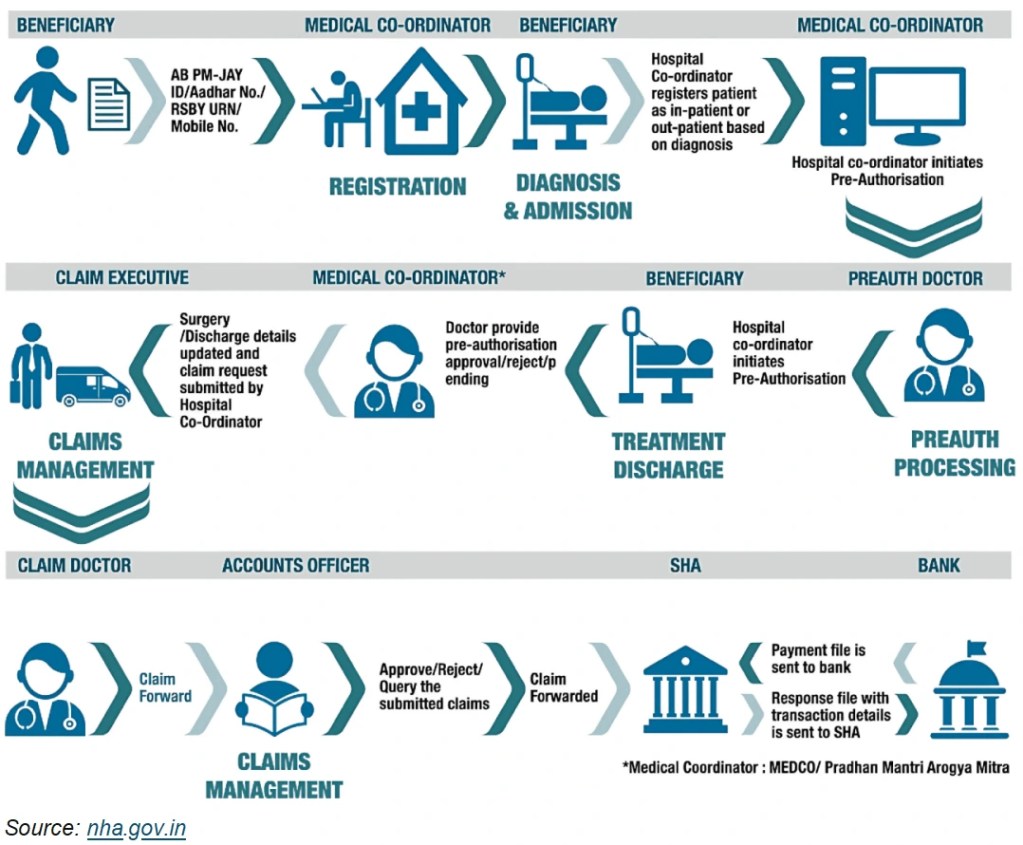
Identification: Families identified via SECC database + state health scheme databases
e-Cards Issued: Beneficiaries receive a digital Ayushman card
Hospital Network: 26,000+ empanelled hospitals (public and private)
Claims Settlement: Done digitally through TPA or insurance partner, monitored National Health Authority (NHA)
Tech Backbone: Includes Health ID (ABHA), Hospital Management Info Systems, and real-time dashboards
Impact:
- Over 6 crore hospitalizations processed
- ₹75,000+ crore worth of treatments funded
- Major private hospital chains participate (Apollo, Max, etc.)
Pradhan Mantri Fasal Bima Yojana (PMFBY):
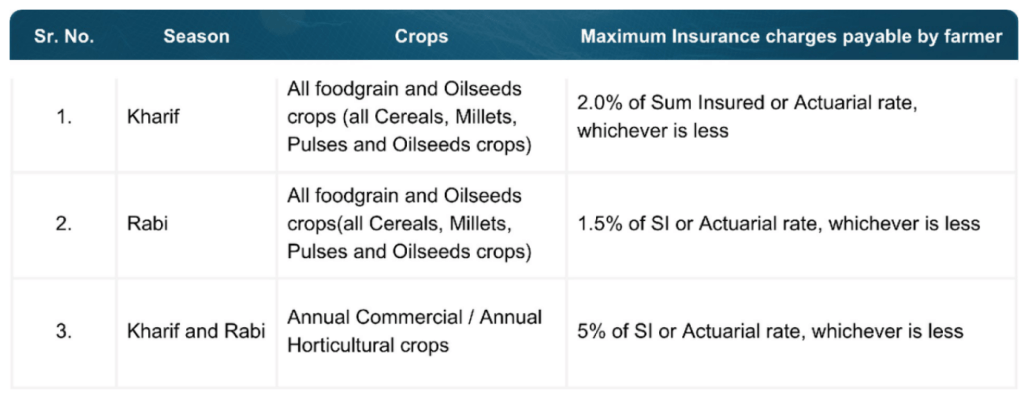
In the domain of agricultural risk mitigation, the Pradhan Mantri Fasal Bima Yojana (PMFBY) serves as a critical safety net for India’s farmers. Launched in 2016, the scheme insures farmers against crop loss arising from natural calamities such as floods, drought, and pest infestations. It covers food grains, oilseeds, and commercial crops, offering heavily subsidized premiums—with farmers contributing only 1.5% to 2% of the sum insured. Enrollment is facilitated through banks, Common Service Centres (CSCs), and digital portals, and the scheme is supported by a sophisticated assessment framework using satellite imaging, drone technology, and localized weather data. Claims are settled directly into the farmer’s Aadhaar-linked bank account via the Direct Benefit Transfer (DBT) system. PMFBY currently reaches approximately 5–6 crore farmers annually and has disbursed over ₹1.15 lakh crore in claims. Participating insurers include both public and private players such as the Agriculture Insurance Company of India (AIC), HDFC ERGO, and IFFCO Tokio.

Overall Statistics
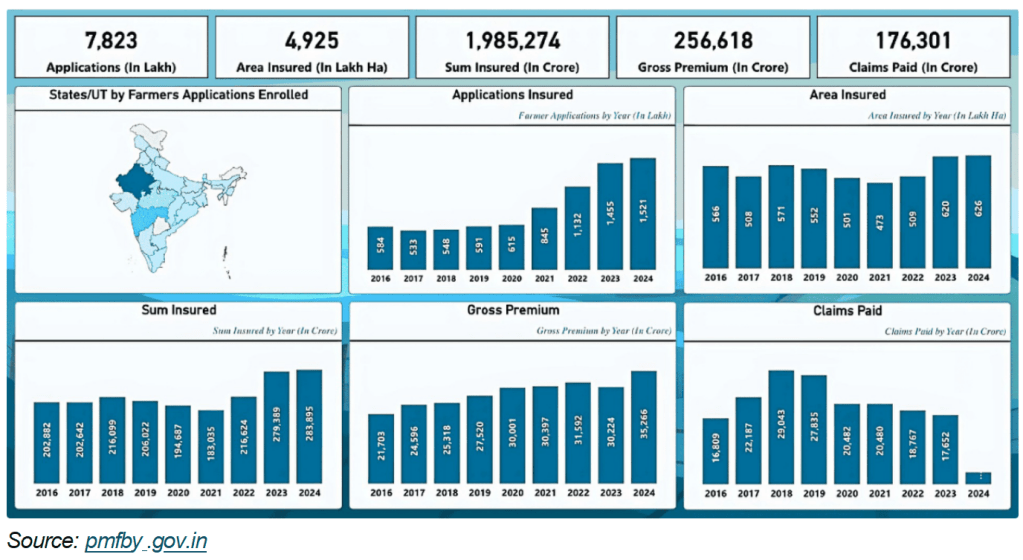
Impact
- Covers 5–6 crore farmers annually
- ₹1.15 lakh crore paid out in claims (as of 2023)
- Participating insurers: IFFCO Tokio, HDFC ERGO, Agriculture Insurance Company of India (AIC), etc.
Jan Suraksha Schemes:
At the microinsurance level, schemes like PMJJBY (life insurance) and PMSBY (accidental insurance) make basic risk cover available to millions of low-income earners. Priced at ₹330/year and ₹12/year respectively, they offer ₹2 lakh in coverage and are linked directly to bank accounts. Enrollment and premium payment are automated through the NACH platform, and claims can be processed via local bank branches. LIC and several private insurers handle policy issuance and claims processing. These schemes have seen more than 40 crore enrollments and have become essential risk cushions for daily-wage workers, gig economy participants, and small traders.
Infrastructure & Delivery Mechanisms:
The success of these schemes is underpinned by India’s robust digital public infrastructure. Aadhaar authentication ensures accurate beneficiary identification and eliminates duplication. The integration of Jan Dhan bank accounts with national payments systems enables frictionless premium collection and claim disbursement. Real-time dashboards, centralized policy management systems, and API-based integrations with insurance companies ensure operational efficiency and transparency across the ecosystem. The roles played by public sector banks, insurance companies, third-party administrators (TPAs), and government agencies are tightly interlinked to support last-mile delivery at scale.
Challenges & Gaps in Execution:
Despite their achievements, these initiatives are not without challenges. Gaps in awareness persist among eligible beneficiaries, and delays in claim processing— particularly under PMFBY during widespread natural disasters—continue to pose operational difficulties. Additionally, the dependence on legacy data like SECC 2011 has led to issues in targeting and coverage accuracy, while some state-level variations in scheme adoption affect uniformity in nationwide implementation.
Read more

Usage-Based Motor Insurance & Telematics in India: The Next Wave
Telematics and data-driven pricing are transforming India’s motor insurance bringing fairer, personalised, and smarter coverage for modern drivers.

AI-Powered Compliance: How RegTech is Transforming Insurance Governance
Discover how AI-driven RegTech is reshaping insurance compliance in India from DPDPA readiness to real-time, automated governance and risk management.

DPDPA Meets AI: Regulating the Future of Intelligent Insurance
Learn how DPDPA reshapes AI in insurance from consent and data ethics to bias and explainability defining a new era of responsible innovation.



